STAR HIE Program Helps Unlock Powerful Public Health Data in West Virginia
Sonia Chambers; Kevin Eike; Larry Jessup and LaVerne Perlie | November 29, 2022
ONC launched the Strengthening the Technical Advancement and Readiness of Public Health Agencies via Health Information Exchange (STAR HIE) Program in 2020 using funding from the Coronavirus Aid, Relief, and Economic Security Act (CARES Act). The program was expanded in 2021 to increase support for efforts to improve vaccination data sharing between jurisdictional Immunization Information Systems (IIS) and HIEs. The West Virginia Health Information Network (WVHIN) was among the 22 recipients that received a combined $20 million in funds from ONC via the CARES Act.
We sat down with WVHIN’s Executive Director, Sonia Chambers, to learn how the STAR HIE Program helped WVHIN support the state’s public health agency exchange health information during the COVID-19 pandemic. (Answers have been edited for clarity.)
What was the STAR HIE Program funding used for?
ONC’s STAR HIE Program really served as a catalyst for much of our COVID-19 activities, both through the direct funding and by creating a closer relationship between the WVHIN and the state’s Bureau for Public Health. In fact, the Bureau for Public Health were the ones who noticed the STAR HIE Program Request for Proposal (RFP) and sent it to us. That engagement between us and the Bureau for Public Health sparked greater coordination and collaboration which has further increased during the pandemic.
The STAR HIE Program enabled us to create two important tools to assist with COVID-19 vaccine tracking and outreach: (1) The ImmuTrack tool to support providers and payers, and (2) the WVHIN Reporting Services Heat Maps to support public health officials. The ImmuTrack tool enables providers to view their entire patient panel and the vaccination status of those patients in one document. The tool is searchable by dose, age, geography, race, and ethnicity and includes chronic conditions for Medicaid patients. The same data can be fed into more sophisticated systems. Previously, providers had to query the state’s IIS on a patient-by-patient basis, which is incredibly tedious and slow.
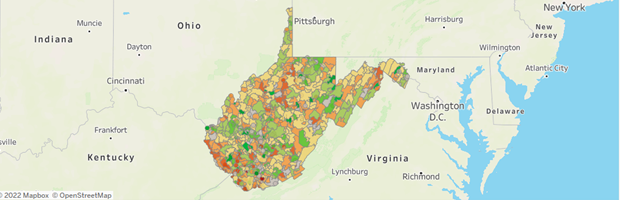
The WVHIN Reporting Services Heat Maps display vaccine data at a population level and may be customized in various ways, including by county, ZIP code, Census Tract, age, race, ethnicity, Centers for Disease Control and Prevention (CDC) Agency for Toxic Substances and Disease References (ATSDR) Social Vulnerability Index, by total number or percentage compared to averages, and more. As you can imagine, these types of maps have been very helpful in targeting vaccine outreach efforts. The resulting reports have been used by the WV Bureau for Public Health, regional epidemiologists, local health departments, Federally Qualified Health Center (FQHCs), the Partnership for African American Churches (PAAC) and higher education.
Both of those tools were critical to the state’s being better prepared to deal with COVID-19 as the pandemic unfolded.
FIGURE 1: Unvaccinated individuals by county
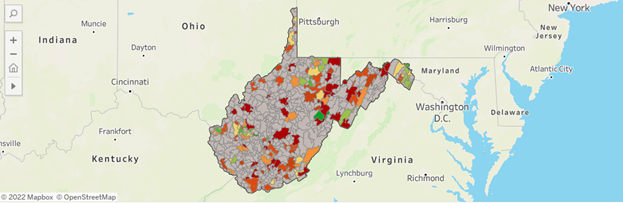
FIGURE 2: Unvaccinated, Black individuals by county
What problems/challenges existed and how did the STAR HIE Program funding help?
We had several challenges. When COVID-19 first hit West Virginia, only four hospitals or hospital systems in the state were reporting COVID-19 lab results to the state electronically. We had been working with them on connecting to the Electronic Lab Reporting (ELR) program, but West Virginia’s ELR certification process is lengthy, taking several months to complete, and many hospitals had other priorities related to technology. Thanks to WVHIN’s existing, strong relationships with hospitals, we were able to partner with the state public health agency to stand up 21 COVID-19-only lab feeds in hospitals in just two short weeks. We’re now working on expanding those feeds to full ELR feeds so that we are better prepared for the next large outbreak.
Another challenge was race and ethnicity identification. It’s clear that minority populations are more likely to be disproportionately impacted by COVID-19 and in the immediate scramble to conduct as many tests as possible when the pandemic first started, race and ethnicity information was often not captured. However, we were able to leverage demographic data from WVHIN’s existing hospital and provider data feeds, which we call our Master Patient Index (MPI), to help the state reduce the percentage of unknown race and ethnicity classification by half! We are also providing this function for vaccine distribution. The WVHIN Reporting Services Heat Maps were and continue to be instrumental in pinpointing areas that are lagging in terms of vaccination rates. This enables us to work directly with community organizations like the PAAC to engage communities of color and identify high-risk patients who have not yet received a vaccination.
Data cleanliness is another persistent challenge since data is often incomplete or frequently changes. For example, many West Virginia residents travel to a bordering state like Ohio for care and vice versa. If a West Virginia resident were to get a vaccination at a Walgreens in Ohio, that could pose challenges with incomplete or even duplicate data. Our MPI continues to be instrumental in matching vaccination data that’s inaccurate or incomplete, and/or merging duplicated entries.
How will you build on this work and what are some future projects for WVHIN?
We’re planning to expand ImmuTrack for use beyond COVID-19 vaccines since it may be useful for other vaccinations like monkeypox or even childhood vaccines. We’ll also build out the heat maps to policymakers and public health officials to better understand gaps in vaccination status relative to geographic location.
Not only was the STAR HIE Program funding instrumental in catalyzing our COVID-19 activities, it also enabled us to demonstrate progress which led to us receiving two additional CDC grants, (1) The National Initiative to Address COVID-19 Health Disparities Among Populations at High-Risk and Underserved, Including Racial and Ethnic Minority Populations and Rural Communities grant and (2) The Vaccination Equity and Prioritizing Populations Disproportionately Affected by COVID-19 grant, to continue our work. Furthermore, we are continuing to work with public health officials and with IIS on data clean-up as part of the Immunization Data Exchange, Advancement and Sharing (IDEAS) collaborative. We’re also leveraging CDC health disparities and vaccine equity grants to provide analytics on things like breakthrough cases and reinfection rates. Additionally, we’re providing automated reports that combine vaccine status, positive COVID-19 tests post-vaccination, deaths, and any relevant inpatient or outpatient visits.
We’re also exploring some work related to social determinants of health (SDOH), specifically being able to show referrals to community-based organizations for things like food insecurity, transportation insecurity, etc. Ultimately, that work seeks to close the referral loop and give more context about a patient’s overall situation to a patient’s care team.
What role do you think HIEs play in improving health?
Our experience in supporting the state’s Bureau for Public Health with COVID-19 response showed us that HIEs are well-positioned to bridge the gaps within our current nationwide public health infrastructure. I think the biggest thing we were able to show is that HIEs are nimble and flexible, two attributes which are absolutely critical in a time of crisis like a global pandemic.
HIEs have existing connectivity and strong data and analytic capabilities which many local governments don’t have. HIEs also have the ability to backfill patient matching and data cleaning. For example, if someone moves and subsequently changes their name, we can help figure that out. One other thing is the ability of HIEs to not only support public health agencies to access data but also then provide that data back to providers to improve patient care. HIEs play a uniquely important role.
Learn more about WVHIN. Learn more about ONC’s STAR HIE Program.