Background
Accurately and consistently matching patient data both within and across organizations is pivotal to ensuring safe and effective care to patients. When patient data is not accurately matched, treatment and diagnosis decisions are made in the absence of valuable information, and patients could be subject to adverse events and significant harm1. To facilitate the best possible treatment and care coordination among a care team, exchanging and linking patient data from across the care continuum is critical.
Patient demographic data is the primary reource used for matching patient records. Unfortunately, patient demographic data is often of poor data quality, resulting in both inaccurate matching of patient records and low match rates, particularly when data is exchanged across organizations. Over the last few years, the industry has considered a number of solutions to help address the problem, including:
- Capturing critical identity attributes to ensure patient identity integrity in any context;
- Adding data elements to the core set of name, address, and data of birth;
- Standardizing terms, definitions, values, formats, and lengths for demographic attributes across the industry;
- Employing matching algorithms that will identify candidate matching records that will compensate for the lack of standards in existing data stores;
- Standardizing best practices for patient registration to ensure quality data is present from the point of entry; and
- Defining and adopting standards for data, and implementing sound data management processes requires increased awareness, effective collaboration, and a cultural evolution towards shared responsibility, both within and across health care organizations.
To support these goals, the Office of the National Coordinator for Health Information Technology (ONC) worked with the CMMI Institute to develop the Patient Demographic Data Quality (PDDQ) Framework. The goal of the PDDQ Framework is to help organizations ensure that formulation, agreements, approvals, and implementation of adopted standards and processes will be effective and sustainable and support the minimization of the number of duplicate records across the industry, ultimately improving patient safety.
About the PDDQ Framework
The PDDQ Framework allows organizations to evaluate themselves against key questions designed to foster collaborative discussion and consensus among all involved stakeholders. Its content reflects a path that organizations can follow when building proactive, defined data quality processes to positively influence behavioral changes in the management of patient demographic data.
The PDDQ Framework enables organizations to quickly assess the current state of data management practices, discover gaps, and formulate actionable plans and initiatives to improve management of the organization’s data assets across functional, departmental, and geographic boundaries. The PDDQ Framework is designed to serve as both a proven yardstick against which progress can be measured as well as an accelerator for an organization-wide approach to improving data quality. If posed to key stakeholders, producers, and consumers of patient demographic data, its 76 questions can stimulate knowledge sharing, surface issues, and provide an outline of what the organization should be doing next to more effectively manage this critical data.
The PDDQ Framework is derived from the Data Management Maturity (DMM)SM Model2, created by the CMMI Institute as a comprehensive reference model of fundamental data management practices. The DMM defines the business processes and specific practices that increasingly lead to greater capabilities and maturity. It contains six categories, 25 process areas, 414 functional practices, and 596 work products. Results from evaluations employing the PDDQ Framework, focused on critical patient demographic data, are intended to align with those that would be produced from employing the full DMM.
The PDDQ Framework addresses practical, proven activities needed to achieve and sustain effective management of an organization’s patient demographic data. It incorporates best practices designed to help the organization establish, build, sustain and optimize effective data management across the patient demographic data lifecycle, from initial creation through updating, delivery, use, and archiving or destruction. It also helps to increase an organization’s appreciation for the criticality of its data assets by engaging staff in increasing capabilities and adopting disciplined practices.
The PDDQ Framework advocates organization-wide alignment on the following key factors:
- Implementing governance functions;
- Planning data quality;
- Implementing quality improvements and assurance;
- Managing operational components;
- Defining and mapping data dependencies;
- Supporting access to shared data interoperability; and
- Ensuring that data is understood and trusted across the organization.
While the PDDQ Framework addresses and advocates requirements and activities for effective data management, it does not prescribe how an organization should achieve these capabilities. It can be used by organizations both to assess their current state of capabilities and build a customized roadmap for data management implementation.
Audience
The expected audience for the PDDQ Framework includes all health care organizations interested in evaluating and improving patient demographic data management by adopting a coordinated, organization-wide approach to achieve accurate, trusted data and reduce record duplication rates.Assessing data management capabilities is a strategic initiative which can yield significant benefits over time. Evaluating current practices against the PDDQ Framework reveals numerous actionable, tactical initiatives that can be accomplished by leveraging existing strengths and making practical, sensible modifications to existing processes. The PDDQ Framework may be applied as a whole or in part, depending on the priorities of the organization. The framework’s embedded outline of successive improvement steps guides implementers in their work to establish and roll out activities needed to achieve and benefit from effective data management practices.
PDDQ Framework
The PDDQ Framework is comprised of five primary categories, illustrated in Figure 1. Each category contains a number of process areas, 19 in all, illustrated in Figure 2.
Figure 1: Patient Demographic Data Quality Framework Category Relationship
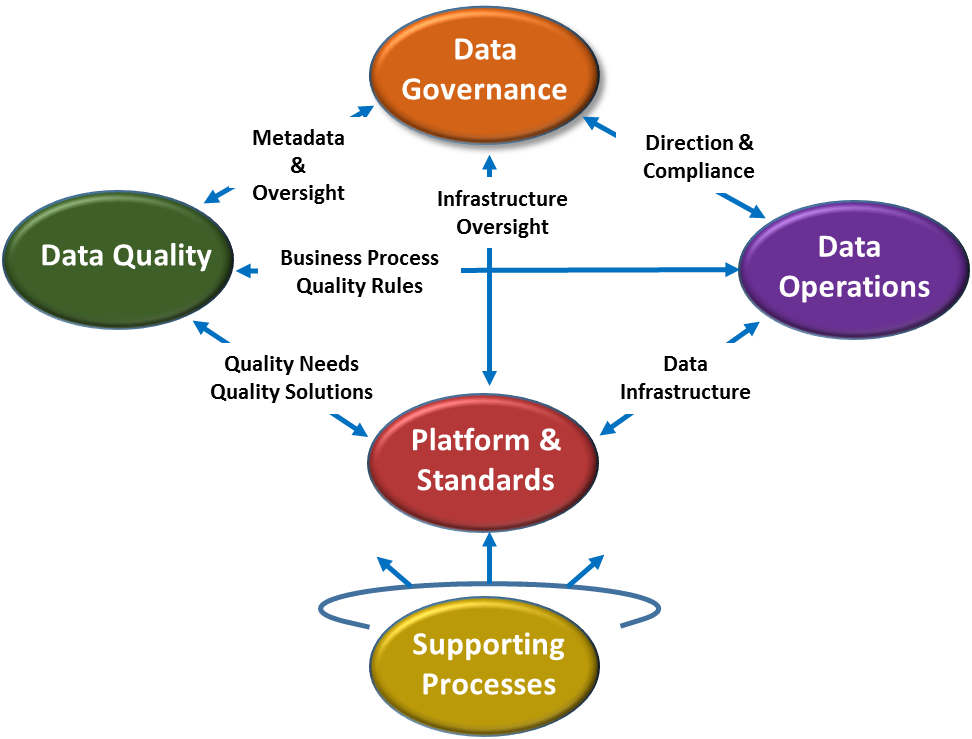
Figure 2: Patient Demographic Data Quality Framework Process Area Organization

Process areas serve as the principal mechanisms to communicate the themes, context, benefits, and example work products of the model, focused around the key evaluation questions contained within each section. Fulfilling practices assists an organization to chart its path and progress in building capabilities.
The PDDQ Framework is structured such that an organization can implement any combination of categories or process areas and obtain baseline conclusions about their capabilities. The organization can focus on a single process area, a set of process areas, a category, a set of categories, or any combination up to and including the entire PDDQ Framework. This allows application to meet specific needs.
Framework Organization
Although each process area can be considered separately, the collection of practices across process areas work together to ensure that the organization has comprehensively addressed fundamental data management best practices. Process area relationships and dependencies exist but are not explicit, because each process area is designed to be evaluated individually; however, these relationships are addressed in supporting informative text and also implied by the collective example work products.
Each process area is composed of the same components, as illustrated in Figure 3.
Figure 3: Process Area Components
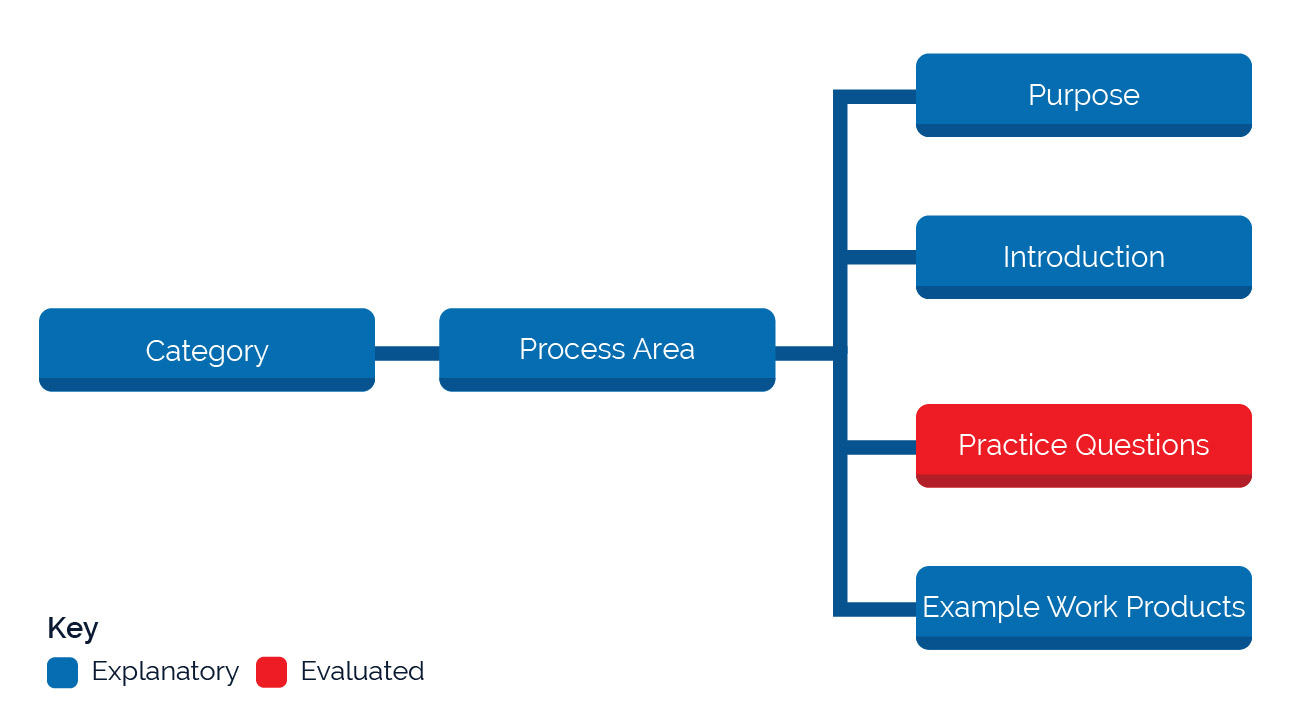
For evaluation purposes, only consensus answers to the key questions are recorded and scored in the accompanying scoring spreadsheet. The introduction to each process area and the explanatory content following the key questions provide additional context for which to interpret the question.
Collectively, the existence of work products helps the organization to determine the extent to which processes are defined and being followed. The example work products provide insight into typical artifacts – documents, templates, mechanisms, metrics, etc. – which are created as processes are developed, established, maintained, and improved. They are presented as helpful examples for the organization to consider. Key questions, reflecting capabilities within a process area, are organized in successive levels of achievements, synthesized from the experience of hundreds of organizations over the past three decades. The PDDQ Framework organizes these progressive levels in ‘Tiers.’ Tier 1 Foundational address capabilities that are typically accomplished first, Tier 2 Building questions target capabilities that build on the foundation of Tier 1, and Tier 3 Advanced features capabilities that comprise completion of the practices necessary for a sound and sustainable program for managing patient demographic data across the lifecycle.
Scoring
In general, a score of 3.0 in any process area indicates that an organization is managing its data very effectively with respect to the featured practices. However, organizations should not be discouraged if the initial score is lower. The intent of the PDDQ Framework can be stated as “Wherever you are, there you are.” It is intended to be an encouraging and helpful mechanism for discovery, to assist organizations on their path to effectively managing patient data. Each question can be answered in three ways: Full means that the organization’s consensus opinion is that it is indeed performing the practices indicated. Partial means the consensus is that portions of the practices are being performed. None means that at the time of the evaluation, the practices indicated by the question are not being performed. Each Tier must be answered as Full to receive the maximum score. If Tier 1 is Partial and Tier 2 is Full, the organization will receive a score of .5 instead of 2.0. However, the organization may discover that the effort to complete Tier 1 is not extensive; in that case, the impact of implementing Tier 1 practices fully would raise the score to 2.0.
References
1 A recent report from the ECRI Institute reviewed more than 7,700 safety-related events that were caused by or related to incorrect patient identification and occurred from January 2013 to August 2015. See the Executive Summary for more information: https://www.ecri.org/Resources/Whitepapers_and_reports/PSO%20Deep%20Dives/Deep%20Dive_PT_ID _2016_exec%20summary.pdf
2 The DMM is available from the CMMI Institute https://dmm-model-individual.dpdcart.com/
